Keratoconus Causes & Treatment: What is keratoconus?
Keratoconus is a progressive corneal disease that affects the cornea’s structure and shape, causing blurry and distorted vision. The cornea is the clear outer layer of the eye that protects the eye and allows you to focus and see clearly. As light enters the eye, the cornea refracts the light and focuses it onto your retina. Your retina is your eye’s processing center, helping you make meaning of what you see. For this process to function properly, the cornea must be shaped like a dome to accurately refract light. If the cornea is too steep, flat or asymmetrical, a refractive error results, requiring eyeglasses or contacts to see clearly. Typical refractive disorders include nearsightedness (myopia), farsightedness (hyperopia) and astigmatism.
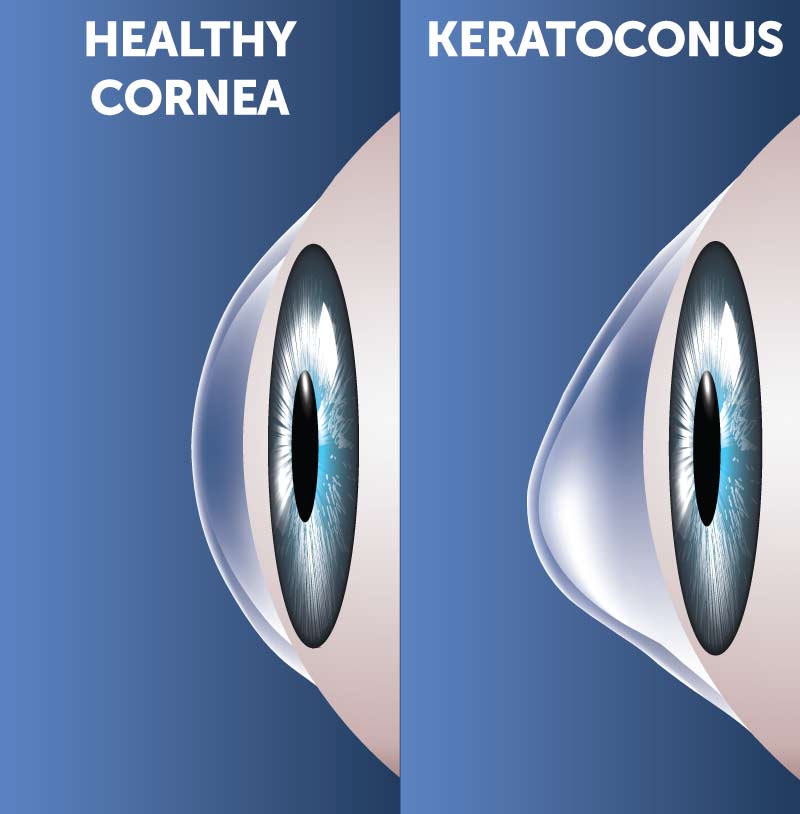
 Unlike typical refractive disorders, keratoconus is the thinning and weakening of the cornea. This change in the cornea’s structural integrity is what progressively reshapes the cornea into a cone-like structure. This abnormal shape causes light to scatter as it enters your eye resulting in distorted and blurry vision. Other symptoms include glare and halos at night and the streaking of lights. Keratoconus is a progressive disease with an average age of onset in the teens or early twenties.
Unlike typical refractive disorders, keratoconus is the thinning and weakening of the cornea. This change in the cornea’s structural integrity is what progressively reshapes the cornea into a cone-like structure. This abnormal shape causes light to scatter as it enters your eye resulting in distorted and blurry vision. Other symptoms include glare and halos at night and the streaking of lights. Keratoconus is a progressive disease with an average age of onset in the teens or early twenties.
How common is keratoconus?
 Keratoconus is more common than originally thought 20 to 30 years ago. As diagnostic testing has become more sensitive and precise, the estimated prevalence of keratoconus in some studies has been shown to be as frequent as one in 375 individuals. In most people who have keratoconus, both eyes are eventually affected, although not always to the same extent. It is not typical for patients to go blind if they have keratoconus, but due to the nature of the disease, vision can be degraded to a level where daily simple tasks such as driving a car or reading a book can become difficult.
Keratoconus is more common than originally thought 20 to 30 years ago. As diagnostic testing has become more sensitive and precise, the estimated prevalence of keratoconus in some studies has been shown to be as frequent as one in 375 individuals. In most people who have keratoconus, both eyes are eventually affected, although not always to the same extent. It is not typical for patients to go blind if they have keratoconus, but due to the nature of the disease, vision can be degraded to a level where daily simple tasks such as driving a car or reading a book can become difficult.
Keratoconus can be a scary thought, but at Wolfe Eye Clinic our cornea specialists have experience in managing and treating keratoconus and can help to answer your questions about the next steps for your diagnosis.
What causes keratoconus?
While not fully understood, many studies show keratoconus tends to run in families and is linked to an abnormality of collagen in the cornea. Collagen is found throughout the body, especially in connective tissues such as muscles and skin. Made of tiny fibers of protein, collagen in your eye keeps the cornea strong and resistant to a change in its normal shape. In keratoconus, these fibers become thin and weak and are no longer able to adequately support the shape of the cornea.
The tendency to develop keratoconus may be present from birth and it appears to be genetic. However, many patients that develop keratoconus do not have a family history of the disease. If you have been diagnosed, it’s recommended to have your children’s eyes checked starting by age ten. Other risk factors include:
● Eye rubbing
● Chronic eye irritation
● Allergies, asthma and/or eczema (Atopic disease)
● Certain medical conditions such as down syndrome
Keratoconus Treatment
 The best keratoconus treatment depends on the severity of disease at the time of diagnosis. It is highly recommended that all patients diagnosed with keratoconus avoid rubbing their eyes to decrease their risk of progression. Early stages of keratoconus can usually be treated with glasses or hard, gas-permeable contact lenses. As the disease progresses and the corneal shape worsens, eyeglasses may no longer be able to provide clear vision and contacts may no longer fit comfortably. At this point, procedures such as corneal cross-linking or in severe cases, corneal transplants may be considered.
The best keratoconus treatment depends on the severity of disease at the time of diagnosis. It is highly recommended that all patients diagnosed with keratoconus avoid rubbing their eyes to decrease their risk of progression. Early stages of keratoconus can usually be treated with glasses or hard, gas-permeable contact lenses. As the disease progresses and the corneal shape worsens, eyeglasses may no longer be able to provide clear vision and contacts may no longer fit comfortably. At this point, procedures such as corneal cross-linking or in severe cases, corneal transplants may be considered.
Corneal Cross-linking for Keratoconus
Corneal cross-linking is a minimally invasive outpatient procedure offered by Wolfe Eye Clinic in Des Moines and Cedar Rapids (Hiawatha) that helps limit the progression of keratoconus by helping to strengthen the cornea. The cornea maintains its round shape through cross-links between its collagen fibers. In keratoconus, the cornea is weak with too few cross-links or “support beams,” allowing the cornea to bulge outwards into a cone-shape. In order to make the cornea stronger, a cross-linking procedure at Wolfe Eye Clinic uses KXL® System technology and a combination of UVA light and Vitamin B2 (riboflavin) eye drops to add cross-links or “support beams.” This helps the cornea hold its shape, better its focusing power, and slow or stop the disease from further progressing. Research has shown that cross-linking is an effective keratoconus treatment, slowing or stopping the progression of keratoconus in over 95% of patients.
Until recently, patients with keratoconus had no FDA-approved therapeutic options to treat progressive keratoconus. In 2016, the FDA approved the KXL® System and use of UVA light and vitamin B2 eye drops as the first and only way to therapeutically treat progressive keratoconus. Wolfe Eye Clinic introduced this technology to treat keratoconus in Iowa that same year upon FDA approval.
Cross-linking has been studied around the world since the late 1990’s. The safety and efficacy of corneal cross-linking has been shown unanimously in numerous studies throughout the world. In fact, all twenty-five European Union nations had approved the procedure by 2006. Like any surgery, there are risks associated with cross-linking and it works best for patients that are good candidates. Evaluations for corneal cross-linking in Iowa are offered with Wolfe Eye Clinic cornea specialists in Hiawatha (Cedar Rapids) and West Des Moines.
Your Cornea Evaluation at Wolfe Eye Clinic
During your cornea consultation you will undergo advanced testing to identify whether you are a good candidate for cross-linking. Your cornea surgeon will discuss the appropriate options for your treatment and the potential risks, as well as answer any questions you may have. Cornea evaluations require specialized testing by a cornea specialist and can be performed at Wolfe Eye Clinic offices in Des Moines, Fort Dodge, Hiawatha (Cedar Rapids), Iowa City, Marshalltown, Ottumwa and Pleasant Hill. Should it be needed, Wolfe Eye Clinic cornea surgeons perform cross-linking surgery at our Hiawatha (Cedar Rapids) and West Des Moines specialty surgical suites.
Find a Cornea Specialist Near You and Get Keratoconus Treatment
Wolfe Eye Clinic has corneal specialists with expertise in treating keratoconus and performing cross-linking at our Hiawatha (Cedar Rapids) and Des Moines clinics. If you have questions or would like to schedule an appointment with one of our keratoconus specialists, fill out our form here, or give us a call at (833) 474-5850.